I am a neonatologist and clinical researcher at Emory University School of Medicine and Children's Healthcare of Atlanta. My research interests include necrotizing enterocolitis, blood transfusion and caffeine therapy.
Epidemiology of Necrotizing enterocolitis:
The primary focus of my research is to understand the epidemiology of necrotizing enterocolitis. Current studies are investigating US trends in incidence and the role of red cell and platelet transfusions, anemia, probiotics and cytomegalovirus.
Neonatal transfusion:
Working with Dr. Cassandra Josephson, I am studying the role of red cell and platelet transfusion in necrotizing entercolitis and coagulopathy in infants with hypoxic-ischemic encephalopathy.
Caffeine therapy in preterm infants:
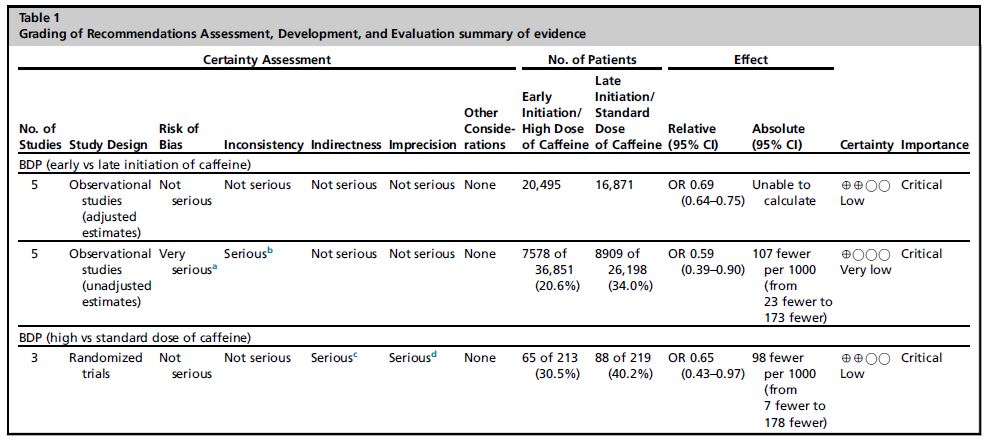
My studies have focused on how to optimze caffeine therapy in preterm infants. My goal is to identify the ideal age at initiation of caffeine to yield the best possible clinical outcomes for preterm infants.
Survival of extremely preterm infants:
In collaboration with investigators in the NICHD Neonatal Research Network, I am interested in understanding the incidence and determinants of survival of extremely preterm infants.
Specific studies related to these projects can be found here.
Current:
Vivek Saroha, MD, PhD - Vivek is interested in the role of very early caffeine use and neonatal outcomes. He is a currently a Assistant Professor of Pediatrics.
Nitya Nair, MD - Nitya is interested in better understanding prognostic discordance in peri-viable birth outcomes.
Mattie Wolf, MD - Mattie is study trends in US necrotizing enterocolitis infant mortality rates and how breastfeeding, povery and racial disparity are associated with geographic differences.
Anand Salem, DO - Anand is interested understanding how peri-extubation caffeine use influences extubation success.
Becca Dryer, MS-4 - Becca is working with Anand on studying peri-extuabtion caffeine use and also evaluating predictors of extubation success.
Prior:
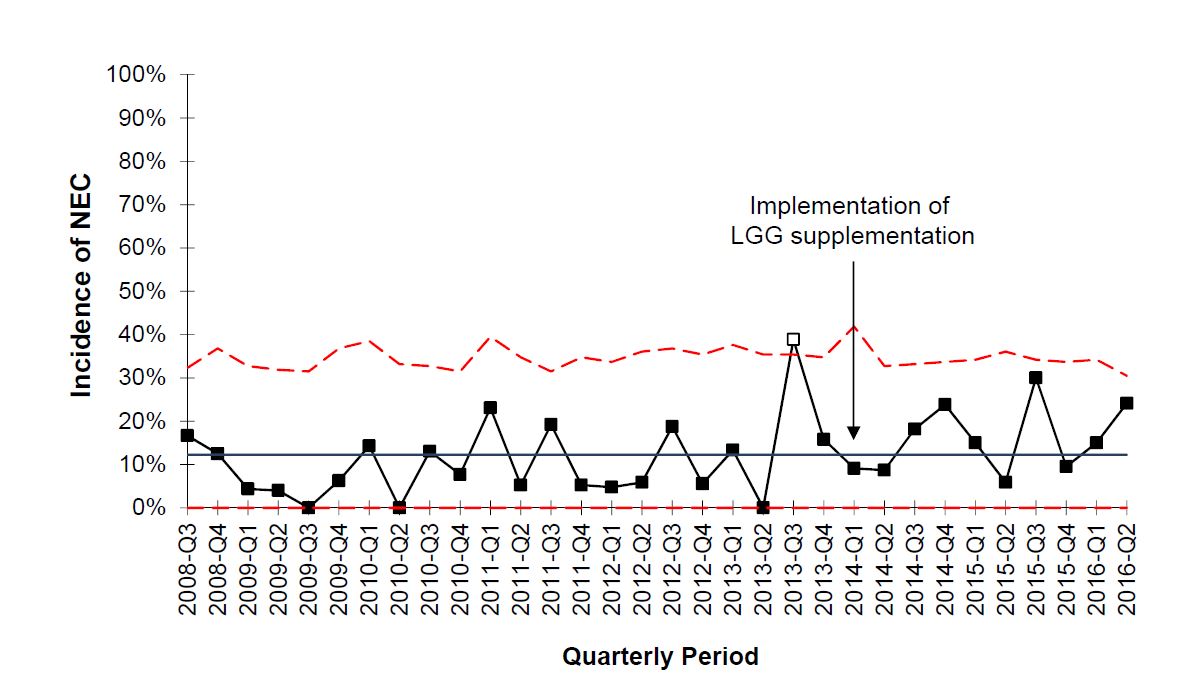
Andrea Kane, MD - Resarch focused on the effectiveness of routine probiotic supplementation to prevent NEC. Current position: Assistant Professor, Wayne State University.
Anisha Bhatia, MD - Research focused on whether implementation of delayed cord clamping can decrease the incidence NEC. Current position: Neonatology fellow, University of Alabama at Birmingham.
Mitali Pakvasa, MD - Research focused on understanding coagulaopahy in infants with hypoxic-ischemic encephalopathy. Current position: Assistant Professor, Emory University.
Tracie Walker, MD - Research focused on early feeding factors influencing exclusive human milk use. Current position, Attending, Children's Healthcare of Atlanta.
Rachel Buckle, MD - Research focused on understanding how early hemodynamic instability ia associated with necrotizing enterocolitis. Current position, Resident in Pediatrics, Brown University.
Mentors:
Cassandra Josephson, MD (mentor for K23 award)
Barbara Stoll, MD
David Carlton, MD
Patricia Denning, MD
Publications (since 2014):
- George L, Menden H, Xia S, Yu W, Holmes A, Johnston J, Reid KJ, Josephson CD, Patel RM, Ahmed A, Mulrooney N, Miller NA, Farrow E, Sampath V. ITGB2 (Integrin β2) Immunomodulatory Gene Variants in Premature Infants With Necrotizing Enterocolitis. J Pediatr Gastroenterol Nutr. 2020 Sep 9.
- Underwood MA, Umberger E, Patel RM. Safety and efficacy of probiotic administration to preterm infants: ten common questions. Pediatr Res. 2020 Aug;88(Suppl 1):48-55.
- Patel RM, Ferguson J, McElroy SJ, Khashu M, Caplan MS. Defining necrotizing enterocolitis: current difficulties and future opportunities. Pediatr Res. 2020 Aug;88(Suppl 1):10-15.
- Rose AT, Saroha V, Patel RM. Transfusion-related Gut Injury and Necrotizing Enterocolitis. Clin Perinatol. 2020 Jun;47(2):399-412.
- Goel R, Josephson CD, Patel EU, Petersen MR, Makhani S, Frank SM, Ness PM, Bloch EM, Gehrie EA, Lokhandwala PM, Nellis MM, Karam O, Shaz BH, Patel RM, Tobian AAR. Perioperative Transfusions and Venous Thromboembolism. Pediatrics. 2020 Apr;145(4):e20192351.
- Rysavy MA, Horbar JD, Bell EF, Li L, Greenberg LT, Tyson JE, Patel RM, Carlo WA, Younge NE, Green CE, Edwards EM, Hintz SR, Walsh MC, Buzas JS, Das A, Higgins RD; Eunice Kennedy Shriver NICHD Neonatal Research Network and Vermont Oxford Network. Assessment of an Updated Neonatal Research Network Extremely Preterm Birth Outcome Model in the Vermont Oxford Network. JAMA Pediatr. 2020 May 1;174(5):e196294.
- Keene SD, Patel RM, Stansfield BK, Davis J, Josephson CD, Winkler AM. Blood product transfusion and mortality in neonatal extracorporeal membrane
oxygenation. Transfusion. 2020 Feb;60(2):262-268. - Patel RM, Josephson C. Neonatal and pediatric platelet transfusions: current concepts and controversies. Curr Opin Hematol. 2019 Nov;26(6):466-472.
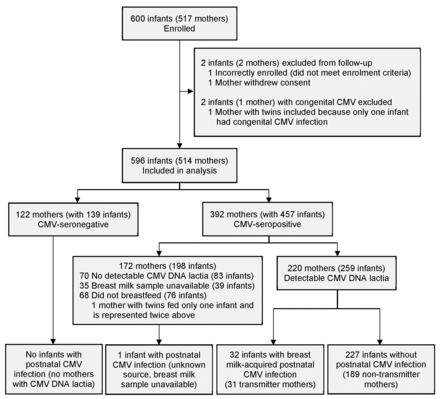
- Patel RM, Shenvi N, Knezevic A, Hinkes M, Bugg GW, Stowell SR, Roback JD, Easley KA, Josephson C. Observational study of cytomegalovirus from breast milk
and necrotising enterocolitis. Arch Dis Child Fetal Neonatal Ed. 2019 Jul 20;105(3):259–65. - Caplan MS, Underwood MA, Modi N, Patel R, Gordon PV, Sylvester KG, McElroy S, Manzoni P, Gephart S, Chwals WJ, Turner MA, Davis JM; Necrotizing Enterocolitis Workgroup of the International Neonatal Consortium. Necrotizing Enterocolitis: Using Regulatory Science and Drug Development to Improve Outcomes. J Pediatr. 2019 Sep;212:208-215.e1.
- Barbian ME, Buckle R, Denning PW, Patel RM. To start or not: Factors to consider when implementing routine probiotic use in the NICU. Early Hum Dev. 2019 Aug;135:66-71.
- Arthur CM, Nalbant D, Feldman HA, Saeedi BJ, Matthews J, Robinson BS, Kamili NA, Bennett A, Cress GA, Sola-Visner M, Jones RM, Zimmerman MB, Neish AS, Patel RM, Nopoulos P, Georgieff MK, Roback JD, Widness JA, Josephson CD, Stowell SR. Anemia induces gut inflammation and injury in an animal model of preterm infants. Transfusion. 2019 Apr;59(4):1233-1245.
- Patel RM, Knezevic A, Yang J, Shenvi N, Hinkes M, Roback JD, Easley KA, Josephson CD. Enteral iron supplementation, red blood cell transfusion, and risk of bronchopulmonary dysplasia in very-low-birth-weight infants. Transfusion. 2019 May;59(5):1675-1682.
- Saroha V, Josephson CD, Patel RM. Epidemiology of Necrotizing Enterocolitis: New Considerations Regarding the Influence of Red Blood Cell Transfusions and Anemia. Clin Perinatol. 2019 Mar;46(1):101-117.
- Jain VG, Saroha V, Patel RM, Jobe A. Is early caffeine therapy safe and effective for ventilated preterm infants? J Perinatol. 2019 May;39(5):754-757.
- Patel RM, Josephson CD, Shenvi N, Maheshwari A, Easley KA, Stowell S, Sola-Visner M, Ferrer-Marin F. Platelet transfusions and mortality in necrotizing enterocolitis. Transfusion. 2019 Mar;59(3):981-988.
- Rose AT, Patel RM. A critical analysis of risk factors for necrotizing enterocolitis. Semin Fetal Neonatal Med. 2018 Dec;23(6):374-379.
- Marin T, Patel RM, Roback JD, Stowell SR, Guo Y, Easley K, Warnock M, Skvarich J, Josephson CD. Does red blood cell irradiation and/or anemia trigger intestinal injury in premature infants with birth weight ≤ 1250 g? An observational birth cohort study. BMC Pediatr. 2018 Aug 11;18(1):270.
- Keir A, Bamat N, Patel RM, Elkhateeb O, Roland D. Utilising social media to educate and inform healthcare professionals, policy-makers and the broader community in evidence-based healthcare. BMJ Evid Based Med. 2018 Jul 26.
- Guo Y, Wang Y, Marin T, Kirk E, Patel RM, Josephson CD. Statistical methods for characterizing transfusion-related changes in regional oxygenation using near-infrared spectroscopy (NIRS) in preterm infants. Stat Methods Med Res. 2018 Jan 1:962280218786302.
- Patel RM, Manuck TA. Collaboratively Understanding and Improving Outcomes for the Mother, Fetus, and Infant. Clin Perinatol. 2018 Jun;45(2):xix-xx.
- Pakvasa MA, Saroha V, Patel RM. Optimizing Caffeine Use and Risk of Bronchopulmonary Dysplasia in Preterm Infants: A Systematic Review, Meta-analysis, and Application of GRADE Methodology. Clin Perinatol. 2018 Jun;45(2):273-291.
- Kane AF, Bhatia D, Denning PW, Shane AL, Patel RM. Routine Supplementation of Lactobacillus rhamnosus GG and Risk of Necrotizing Enterocolitis in Very Low Birth Weight Infants. J Pediatr. 2018 Apr;195:73-79.e2
- Maheshwari A, Patel RM, Christensen RD. Anemia, red blood cell transfusions, and necrotizing enterocolitis. Seminars in Pediatric Surgery. 2018; 27(1):47-51.
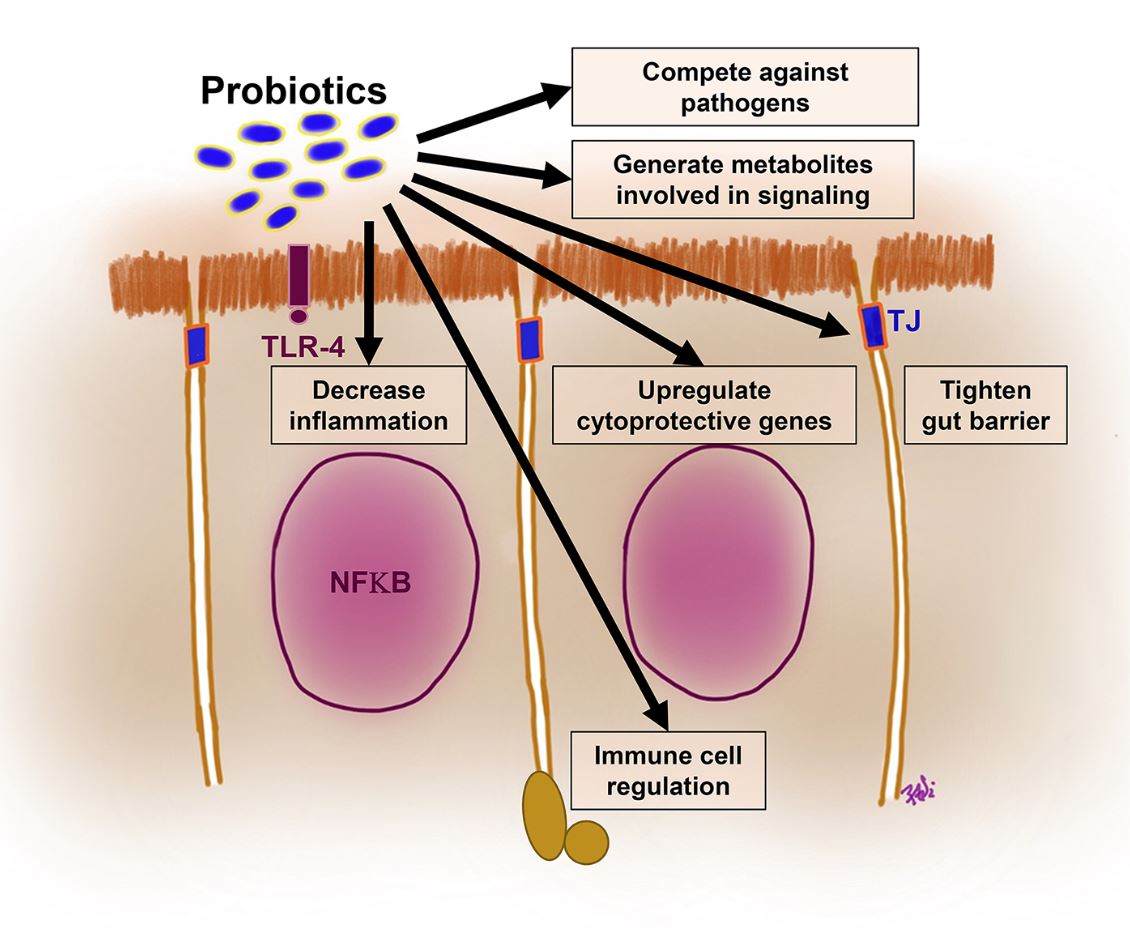
- Patel RM, Underwood MA. Probiotics and necrotizing enterocolitis. Seminars in Pediatric Surgery. 2018; 27(1):39-46.
- Bhatt D, Travers C, Patel RM, Shinnick J, Arps K, Keene S, Raval MV. Predicting Mortality or Intestinal Failure in Infants with Surgical Necrotizing Enterocolitis. J Pediatr. 2017 Dec;191:22-27.e3
- Patel RM, Zimmerman K, Carlton DP, Clark R, Benjamin DK, Smith PB. Early Caffeine Prophylaxis and Risk of Failure of Initial Continuous Positive Airway Pressure in Very Low Birth Weight Infants..J Pediatr. 2017; 190:108-111.e1
- Patel RM, Rysavy MA, Bell EF, Tyson JE. Survival of Infants Born at Periviable Gestational Ages. Clin Perinatol. 2017 Jun;44(2):287-303.
- Younge N, Goldstein RF, Bann CM, Hintz SR, Patel RM, Smith PB, Bell EF, Rysavy MA, Duncan AF, Vohr BR, Das A, Goldberg RN, Higgins RD, Cotten CM; Eunice Kennedy Shriver NICHD Neonatal Research Network. Survival and Neurodevelopmental Outcomes among Periviable Infants. N Engl J Med. 2017 Feb 16;376(7):617-628.
- Patel RM, Meyer EK, Widness JA. Research Opportunities to Improve Neonatal Red Blood Cell Transfusion. Transfus Med Rev. 2016 Oct;30(4):165-73.
- Patel RM, Knezevic A, Shenvi N, Hinkes M, Keene S, Roback JD, Easley KA, Josephson CD. Association of Red Blood Cell Transfusion, Anemia, and Necrotizing Enterocolitis in Very Low-Birth-Weight Infants. JAMA. 2016 Mar 1;315(9):889-97.
- Patel RM. Short- and Long-Term Outcomes for Extremely Preterm Infants. Am J Perinatol. 2016 Feb;33(3):318-28.
- Patel RM, Kandefer S, Walsh MC, Bell EF, Carlo WA, Laptook AR, Sánchez PJ, Shankaran S, Van Meurs KP, Ball MB, Hale EC, Newman NS, Das A, Higgins RD, Stoll BJ; Eunice Kennedy Shriver NICHD Neonatal Research Network. Causes and timing of death in extremely premature infants from 2000 through 2011. N Engl J Med. 2015 Jan 22;372(4):331-40.
- Dobson NR, Patel RM, Smith PB, Kuehn DR, Clark J, Vyas-Read S, Herring A,Laughon MM, Carlton D, Hunt CE. Trends in caffeine use and association between clinical outcomes and timing of therapy in very low birth weight infants. J Pediatr. 2014 May;164(5):992-998.e3.